Flu season here, but outlook uncertain
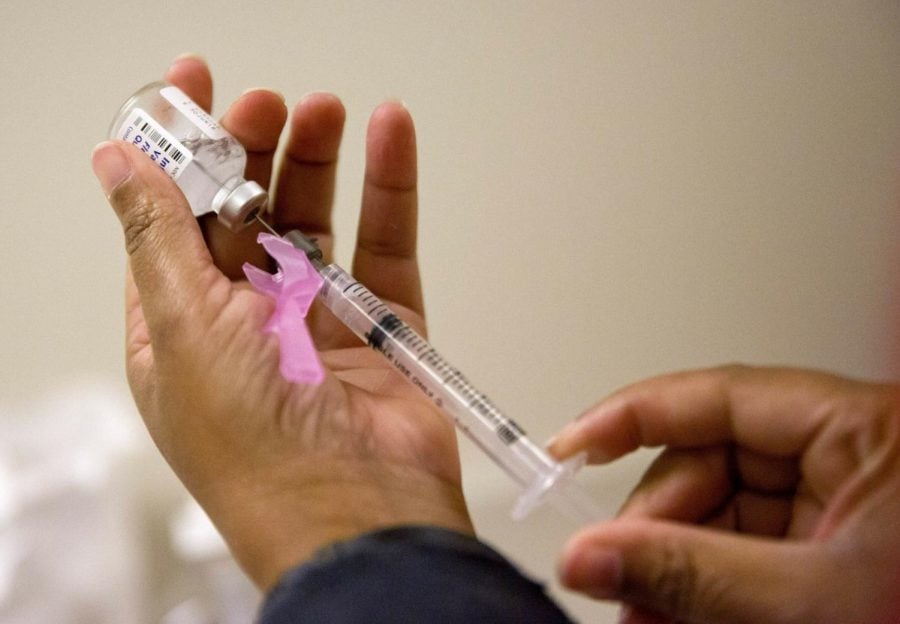
Credit: David Goldman / AP Photo
In this February 7, 2018 file photo, a nurse prepares a flu shot at the Salvation Army in Atlanta.
Fall is here, and that means another flu season is, too. With the 2018-19 flu season being the longest in a decade, bolstered by a second wave of flu that broke out in February, health officials are urging Americans to prepare themselves for the 2019-20 season.
College students are among the groups least likely to get vaccinated, with a vaccination rate between eight and 37 percent, according to a 2017 survey by the National Foundation of Infectious Diseases. The flu season typically begins in fall and goes through winter into the early spring months — sometimes until May. Last year’s flu season lasted 21 weeks, officially ending in mid-April.
The 2017-18 flu season was among the deadliest on record since the CDC began keeping track in 1976. Tens of thousands of people died, including 186 children.
The Centers for Disease Control and Prevention rolled out its annual flu campaign Sept. 26, with Health and Human Services Secretary Alex Azar receiving his own flu shot onstage at a press conference.
A CDC spokesperson told The DePaulia there is no way to predict how a flu season will play out, but people can start preparing now by getting vaccinated and taking preventative measures like washing their hands frequently and covering their mouths when they cough and sneeze. The CDC and Illinois Department of Public Health recommend vaccinations for individuals 6 months and older.
“The amount of flu circulating and the severity depends on the prevalent strains and the match with the vaccine,” IDPH spokesperson Melaney Arnold said in an email. She reiterated the “three C’s”: cleaning hands, covering coughs and sneezes and containing the flu by staying home to prevent the spread of disease.
“Influenza antiviral drugs can be a second line of defense for treatment of some who get sick with the flu,” she added.
Last flu season, 45.6 percent of kids between ages six months to 17 years got vaccinated; the percentage for adults aged 18 and older was 44.9 percent nationally. From October 2018 through May 4, 2019 the CDC estimates between 36,400 and 61,200 people died from the flu.
The flu is caused by the influenza respiratory virus. Flu typically comes on suddenly, with symptoms including fever, head and body aches, coughing, sore throat and runny nose.
While it shares some symptoms with the common cold, flu is much more aggressive and can even result in hospitalization and even death. The most vulnerable populations are infants, pregnant women, the elderly and those with weakened immune systems.
The World Health Organization estimates that 290,000-650,000 people die from influenza-related respiratory deaths every year.
Every year, the updated flu vaccines on offer are designed to combat the most prevalent strains of flu that are in circulation. Strains that this year’s vaccines protect against are A (H1N1), A (H3N2) and B.
Notable outbreaks include the 1918-1919 Spanish flu pandemic, which is estimated to have infected one-third of the world’s population and resulted in 50 million deaths worldwide, and the 2009 H1N1 pandemic, which killed hundreds of thousands and cost the U.S. between $45 and 55 billion.
Last month, an independent group convened by the World Health Organization and the World Bank warned that world governments were not prepared for the next global pandemic. The Global Preparedness Monitoring Group’s report warned that “the world is not prepared for a fast-moving, virulent respiratory pathogen pandemic” and specifically cited the H1N1 pandemic.
In September, President Donald Trump issued an executive order establishing a “National Influenza Vaccine Task Force,” in the hopes of spurring development of a long-sought universal flu vaccine. Such a vaccine could be administered only once, giving long-lasting protection from new and future strains of the flu virus.
Health officials Wednesday confirmed five flu cases in New Mexico, making them the first cases of the 2019-2020 season.
Flu vaccinations in Illinois increased from 35.6 percent to 41.3 percent between the 2017-18 and 2018-2019 flu seasons. Illinois is one of 45 states that allows for religious exemptions to vaccines; 19,000 kids used the religious exemption in the 2018-19 school year.
At DePaul, some students were deciding whether to get vaccinated.
“I might consider taking it, I might not, because I heard you can get sick,” said Ricardo Calderon, a senior studying information technology. “Depending on how I feel that day.”
While soreness and mild fever are sometimes reported by individuals after getting a vaccine, one cannot contract the flu from the flu vaccine. In extremely rare cases, some people have allergic reactions to the vaccine, which can be treated by a doctor.
Karla Marroquin is a senior studying organizational communication. She said she has never caught the flu and does not usually prepare for it.
“The most I do is take Emergen-C and drink tea,” she said.
At the St. Vincent Health Fair on Oct. 21-24, DePaul is offering free flu shots to faculty and staff in partnership with Schaumberg-based Interactive Health.
On Wednesday, DePaul’s Center for Health and Wellness in Lincoln Park had flyers listing flu symptoms and telling students to prevent flu by staying hydrated, washing their hands and getting at least 7 hours of sleep.
“It’s not too late,” the flyer said. “A flu shot could lessen your chances of getting the flu.”